Genes and Medications: How Pharmacogenomics Impacts your Health
What is Pharmacogenomics?
Pharmacogenomics, often referred to as PGx, is the study of how an individual’s genetic makeup or DNA influences their response to drugs. Our genes play a crucial role in determining how our bodies metabolize medications, leading to variations in drug efficacy and safety from person to person.
Sometimes, your genes can make a big difference in how a medication affects you. They could determine whether a drug might cause problems, whether it will work well for you, or if it won’t have any effect at all. What pharmacogenomics does is help you figure all of this out in advance. Armed with this knowledge, your doctor can create personalized treatment plans by choosing the right medication that suits your unique genetic makeup, ensuring it works at its best while keeping you safe and healthy.

How does Pharmacogenomics work?
Medicines work in different ways inside your body, depending on how you take them and where they need to act. After you swallow a pill, your body has to break it down and get it to the right place where it’s supposed to work. Your DNA can actually have a say in how you react to a medicine. Below are a few examples on how the medicines reacts in your body:
EXAMPLES
1. Drug Receptor
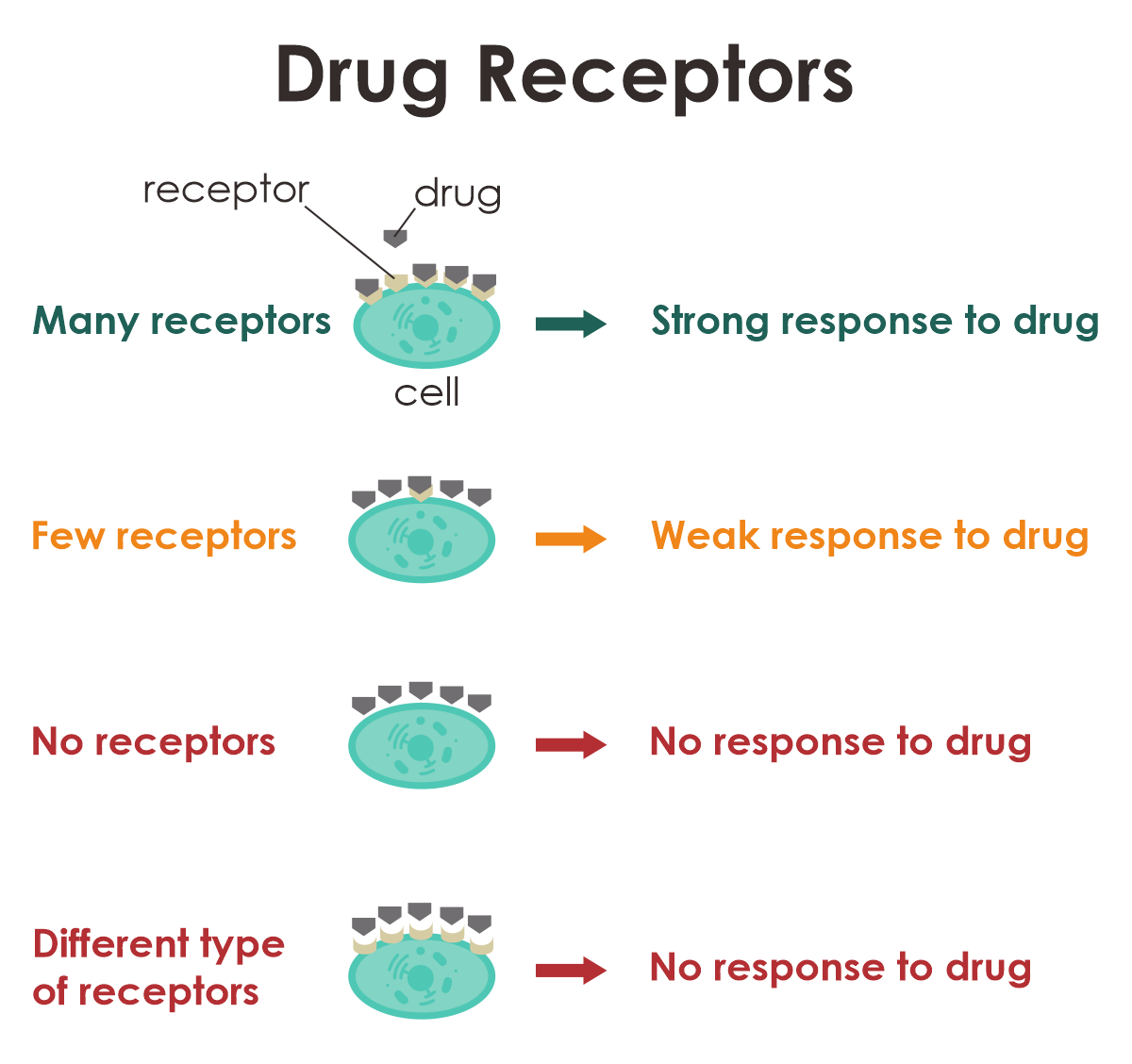
Certain medications require binding to proteins found on the surface of cells, which are known as receptors, to function effectively. Think of medicines as keys, and the receptors as a bunch of locks. Some medicines need to find specific locks on the surface of your cells to work correctly. Your DNA decides what type of locks you have and how many of them. This, in turn, affects how well the medicine works for you. You might need more or less of the medicine than other people, or sometimes, a different medicine altogether might be a better fit for your unique locks.
CASE SCENARIO
Disease: Breast Cancer
Drug: T-DM1
In some cases of breast cancer, there is an excess production of a receptor called HER2, which fuels the growth and spread of the cancer. T-DM1 is a drug specifically designed to combat this type of breast cancer. It does so by binding to the HER2 receptors on cancer cells and effectively eliminating them.
If you have breast cancer, your doctor may analyze a sample of your tumor to determine whether T-DM1 is the appropriate treatment for your condition. If your tumor exhibits a high level of HER2 (HER2 positive), your doctor may recommend T-DM1 as part of your treatment plan. Conversely, if your tumor lacks sufficient HER2 (HER2 negative), T-DM1 would not be effective in treating your cancer.
2. Drug Uptake
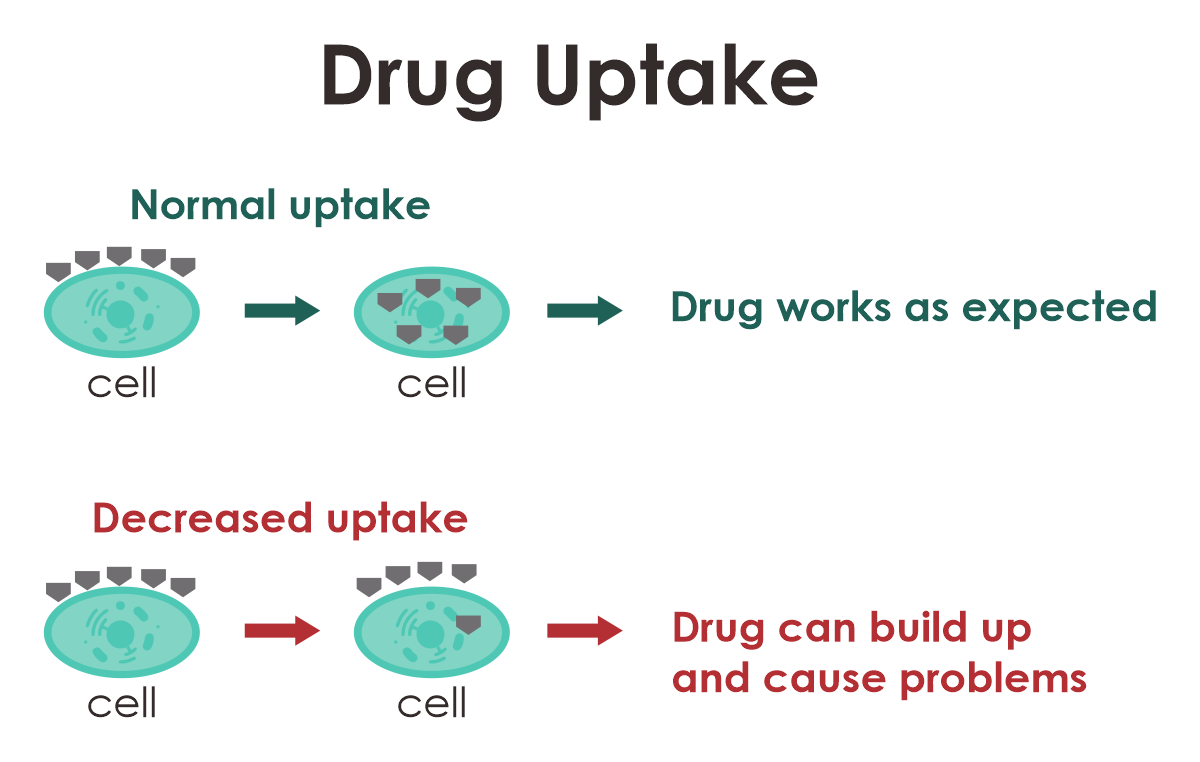
Certain medications require active transport into the specific tissues and cells where they exert their effects. Your DNA can have an impact on the uptake of these drugs. Reduced uptake may result in the medication being less effective and potentially accumulating in other areas of your body, leading to potential issues. Additionally, your DNA can influence the rate at which some drugs are eliminated from the cells where they operate. If these drugs are removed too rapidly from the cells, they might not have adequate time to produce their intended effects.
CASE SCENARIO
Disease: High Cholesterol Level
Drug: Simvastatin (Statin)
Simvastatin is a medication classified as a statin which is commonly prescribed to lower cholesterol levels in the blood. For Simvastatin to function as intended, it needs to be transported into the liver. This transportation process relies on a protein produced by the SLCO1B1 gene. Some individuals possess a specific alteration in this gene, resulting in reduced uptake by the liver. When taken in high doses, simvastatin can accumulate in the bloodstream, potentially leading to muscle-related issues such as weakness and pain.
Before prescribing simvastatin, your doctor might suggest a genetic test to assess the SLCO1B1 gene. This test can help determine if simvastatin is the most suitable statin for your needs or what dose would be the most effective and safe for you.
3. Drug Breakdown
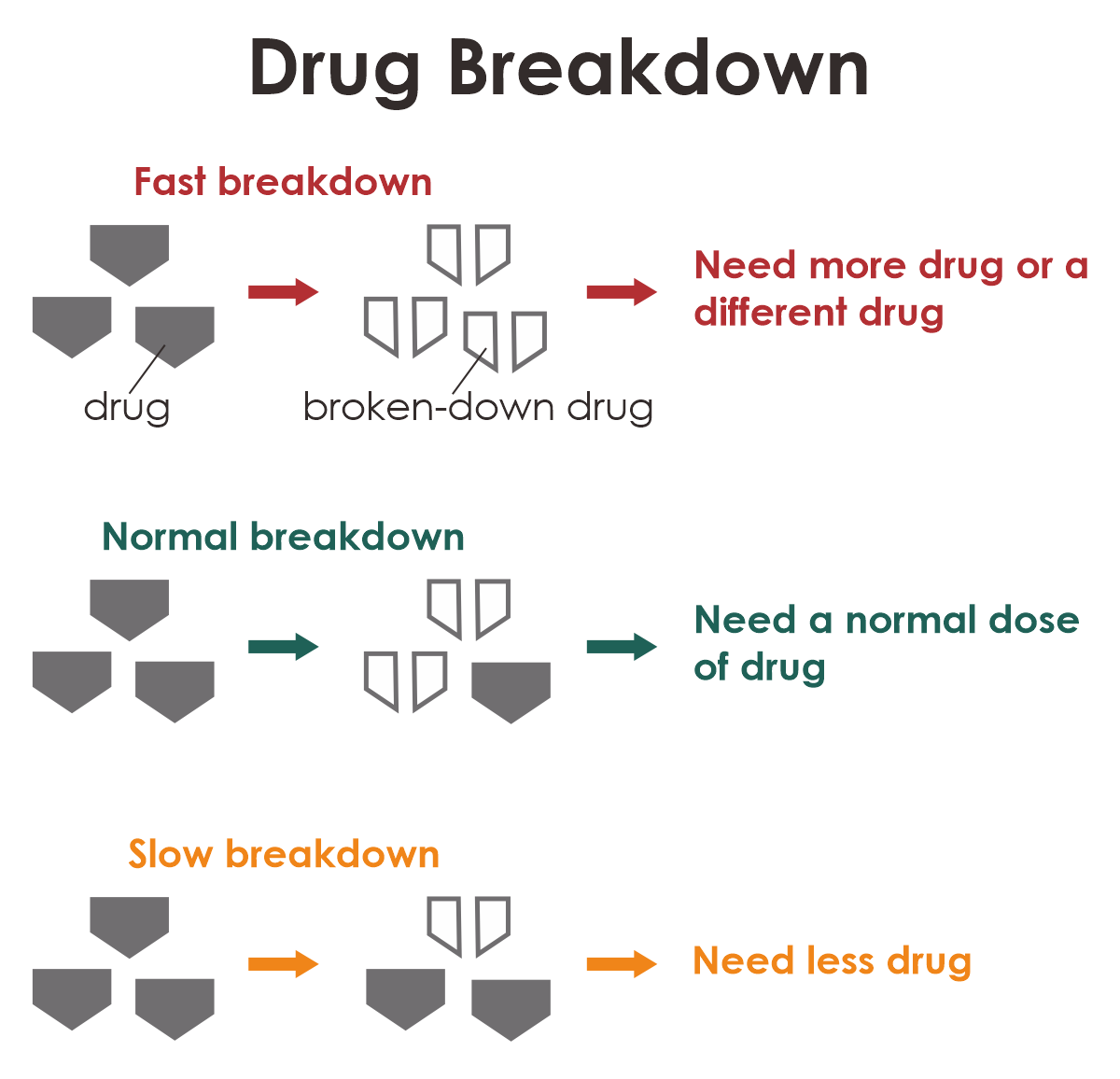
Your DNA can influence the speed at which your body metabolizes a medication. If your body metabolizes the drug faster than the average person, it means your system eliminates the drug more quickly, possibly requiring a higher dosage or a different medication. Conversely, if your body processes the drug more slowly, you may need a lower dose of the medication.
CASE SCENARIO
Disease: Depression
Drug: Amitriptyline
The way your body processes the antidepressant medication amitriptyline depends on the activity of two genes, namely CYP2D6 and CYP2C19. When your doctor prescribes amitriptyline, they may suggest genetic testing for these genes to determine the appropriate dosage for you. If your body metabolizes amitriptyline too rapidly, you might require a higher dose for it to be effective, or your doctor might consider an alternative medication. Conversely, if your body breaks down amitriptyline very slowly, you may need a smaller dose or a different medication to prevent adverse reactions.
4. Targeted Drug Development
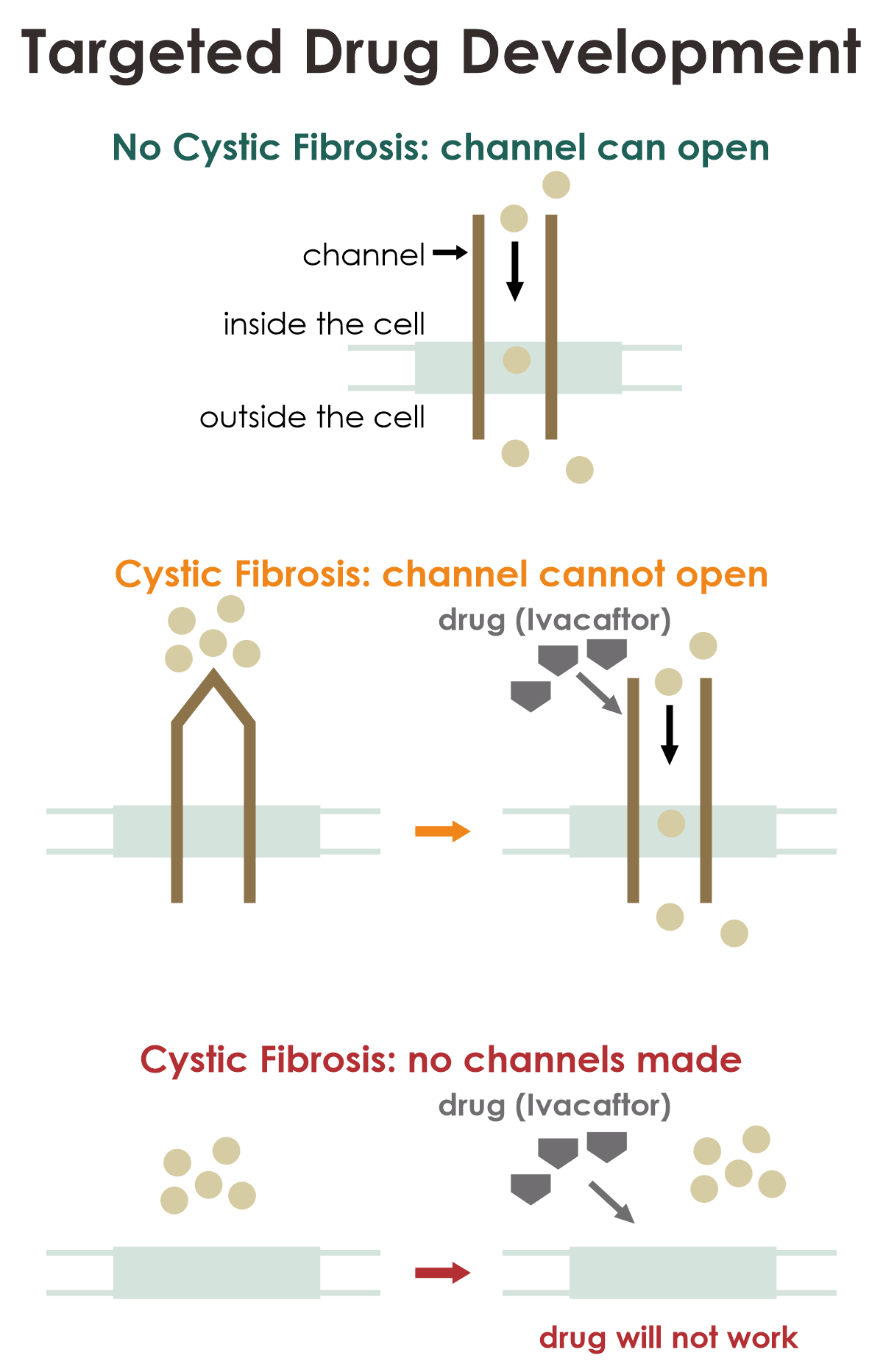
Pharmacogenomic approaches in drug development aim to address the root cause of a condition rather than solely addressing its symptoms. Certain illnesses stem from particular alterations (mutations) in a gene. These mutations can vary, leading to diverse outcomes. Some mutations may lead to a malfunctioning protein, while others might prevent the protein from being produced entirely. Medications can be designed based on how these mutations influence the protein, and these drugs will only be effective for a particular mutation type.
CASE SCENARIO
Disease: Cystic Fibrosis
Drug: Ivacaftor
Cystic fibrosis arises from genetic mutations in the CFTR gene, impacting the functionality of the CFTR protein. This protein serves as a conduit, allowing particles to traverse cell membranes throughout the body. In individuals without cystic fibrosis, the CFTR protein is typically produced correctly, and the channel it forms can open and close as needed.
However, some mutations responsible for cystic fibrosis lead to a closed channel, rendering it nonfunctional. In such cases, the medication ivacaftor intervenes by forcing the channel to remain open. It’s important to note that ivacaftor is not expected to be effective for individuals with cystic fibrosis whose mutations prevent the channel from being produced at all.
SUMMARY
What implications does this have for your well-being?
Pharmacogenomics is a groundbreaking field that has the potential to transform the way we approach healthcare. By tailoring drug treatments to individual genetic makeup, we can improve treatment outcomes, reduce adverse reactions, and enhance overall patient well-being. Initiate a discussion with your healthcare provider regarding the potential impact of pharmacogenomics on your health.

